
What is NPH?
Normal pressure hydrocephalus (NPH) is a form of hydrocephalus that predominantly affects people over the age of 60.
The disease develops gradually. Typical symptoms such as cognitive impairment and urinary incontinence are often mistakenly interpreted as dementia or Alzheimer's disease, or simply put down to old age. However, studies show that around 5% of people diagnosed with dementia actually have NPH.1 Parkinson's-like gait disorders can also lead to misdiagnosis.
NPH Symptoms
If NPH is not diagnosed in time, this generally treatable condition can deteriorate significantly and eventually become irreversible. Early diagnosis and timely treatment can greatly improve patients' chances of returning to a largely normal life.
The pathophysiology (simply: the cause) of NPH is not yet fully understood. Currently, it is thought that it is recurring pressure spikes rather than permanently elevated intracranial pressure that lead to the typical symptoms.3
![[Translate to English:] NPH Symptome Gangbild](/fileadmin/_processed_/4/5/csm_AdobeStock_649532651_square_6a719c6a5b.jpg)
Gait disturbance – often the first symptom
Gait disturbance is usually the earliest and most obvious sign of NPH.
Those affected exhibit a characteristic gait pattern:
- shortened stride length and reduced step height
- wide gait
- outwardly turned toes
- difficulty turning, often requiring five or more steps
- difficulty balancing on one leg or on a line

Cognitive Impairment / Dementia
Typical cognitive symptoms include:
- Concentration problems
- Short-term memory problems
- Psychomotor slowing (slower thinking, speaking and acting)
- Personality or behavioural changes
- Increasing disorientation
Some of these symptoms are similar to those of Alzheimer's disease, which can lead to misdiagnosis.

Incontinence
Urinary incontinence often begins with an urgent need to urinate – a sudden, almost uncontrollable urge to empty the bladder.
Frequency of symptoms



Diagnosis – The earlier, the better!
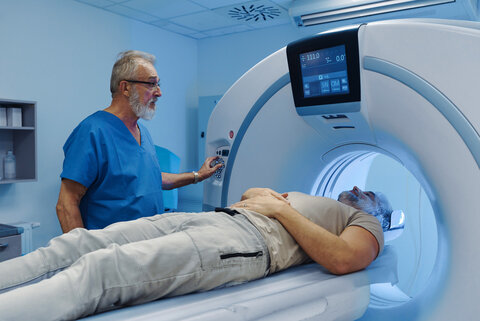
Imaging: MRI and CT
MRI and CT are central to diagnostics.6 These tests can confirm suspicions of NPH by examining whether the ventricles filled with cerebrospinal fluid are enlarged.

NPH Gait Test
In addition to imaging, a short gait test is often carried out. Patients walk ten metres while typical changes are observed. If it takes them more than eight seconds to cover the distance or they take more than 13 steps, this may indicate a gait pattern typical of normal pressure hydrocephalus (NPH). Other signs include significantly shorter step length, a wide gait, and reduced heel lift and roll. Turning on the spot, which often requires five or more steps, and difficulty standing on one leg may also be evident.
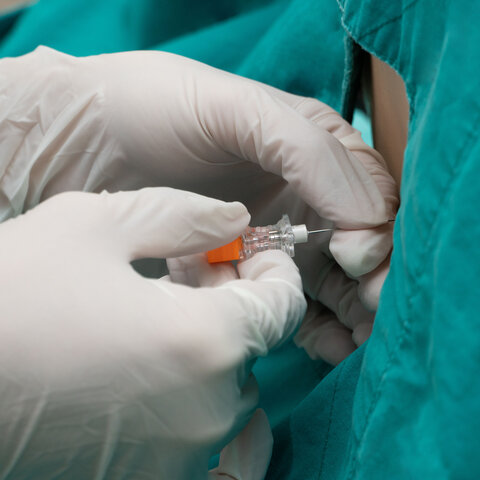
Spinal Tap Test
The spinal tap test (lumbar puncture with cerebrospinal fluid drainage) is used to confirm the diagnosis and assess whether patients would benefit from shunt implantation. The test mimics the effect of a shunt by draining cerebrospinal fluid. For many patients, this results in a significant improvement in symptoms within a short period of time, indicating the potential success of shunt implantation. These improvements begin a few hours after the fluid is removed and can last for several days.
Further Tests
Other commonly used tests include the infusion test, which assesses the ability to break down cerebrospinal fluid, and lumbar drainage, which involves continuously draining cerebrospinal fluid over a period of several days. These procedures complement the diagnostic process and enable a personalised treatment plan to be created.
Treatment of NPH

We Understand the Gravity of the Situation
We believe that responsibility, precision and empathy are all connected. This belief is the reason behind every technical solution we develop. This attitude is reflected in our work every single day.
We develop innovative solutions for people with hydrocephalus, based on our deep understanding of the challenges they face and the requirements of clinical care. Through close partnerships with physicians and the use of precise gravitational technology, we are striving to make treatment safer, more reliable and more successful in the long term.
Our Strong Partner in Neurosurgery:
References
1. Brean A, Fredø HL, Sollid S, et al. Five-year incidence of surgery for idiopathic normal pressure hydrocephalus in Norway. (2009) Acta neurologica Scandinavica, 120(5), 314–316. https://doi.org/10.1111/j.1600-0404.2009.01250.x
2. Nakajima M, Yamada S, Miyajima M, et al. … research committee of idiopathic normal pressure hydrocephalus. Guidelines for Management of Idiopathic Normal Pressure Hydrocephalus (Third Edition): Endorsed by the Japanese Society of Normal Pressure Hydrocephalus. (2021) Neurologia medico-chirurgica, 61(2), 63–97. https://doi.org/10.2176/nmc.st.2020-0292
3. Fritsch MJ, Kehler U, Meier U. NPH – Normal Pressure Hydrocephalus: Pathophysiology – Diagnosis – Treatment. 1st ed. Stuttgart: Georg Thieme Verlag; 2014.
4. Hashimoto M, Ishikawa M, Mori E, et al. Diagnosis of idiopathic normal pressure hydrocephalus is supported by MRI-based scheme: a prospective cohort study. (2010) Fluids Barriers CNS 7, 18. https://doi.org/10.1186/1743-8454-7-18
5. Andrén K, Wikkelsø C, Hellström P, et al. Early shunt surgery improves survival in idiopathic normal pressure hydrocephalus. (2021) European journal of neurology, 28(4), 1153–1159. https://doi.org/10.1111/ene.14671
6. Illies T, Eckert B, Kehler U. What Radiologists Should Know About Normal Pressure Hydrocephalus. (2021) Fortschr Röntgenstr; 193: 1197–1206.


